Rheumatoid Arthritis

Rheumatoid Arthritis
What is rheumatoid arthritis?
Rheumatoid arthritis is a condition that can cause pain, swelling and stiffness in joints.
It is known as an autoimmune condition. This means that the immune system, which is the body’s natural self-defence system, gets confused and starts to attack your body’s healthy tissues. In rheumatoid arthritis, the main way it does this is with inflammation in your joints.
It can affect anyone of any age. It can get worse quickly, so early diagnosis and intensive treatment are important. The sooner you start treatment, the more effective it’s likely to be.
If you have rheumatoid arthritis, your immune system can cause inflammation inside a joint or a number of joints. Inflammation is normally an important part of how your immune system works.
It is not the only disease of joints but it can also involve multiple other organs or system in the body. It affects approximately 1% of the population.
What are the causes of rheumatoid arthritis?
The following can play a part in why someone has rheumatoid arthritis:
Age, Sex, Genetics, Weight, Smoking, Diet
What are the causes of rheumatoid arthritis?
The main symptoms of rheumatoid arthritis are:
- Joint pain
- Joint swelling, warmth and redness
- Stiffness, especially first thing in the morning or after sitting still for a long time.
Other symptoms can include:
- Tiredness and lack of energy – this can be known as fatigue
- Not feeling hungry
- weight loss
- A high temperature, or a fever
- Sweating
- Dry eyes – as a result of inflammation
- Chest pain – as a result of inflammation.
How is it diagnosed?
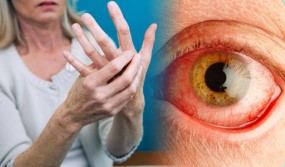
A diagnosis of rheumatoid arthritis is based on your symptoms, a physical examination and the results of x-rays, scans and blood tests.
Because rheumatoid arthritis can affect other parts of the body, it’s important to tell your doctor about all the symptoms you’ve had, even if they don’t seem to be related.
- Blood tests
- X-rays and other tests
- Painkillers
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Disease-modifying anti-rheumatic drugs (DMARDs)
- Steroids
What treatments are there?
There are a variety of treatments available for rheumatoid arthritis.The earlier that intensive treatment is started, the more likely it is
to work.
There are three main ways to treat rheumatoid arthritis:
- Drugs
- Physical Therapies
- Surgery
- CMC
How will rheumatoid arthritis affect body?
Because rheumatoid arthritis can affect different people in different ways, we can’t predict how the condition might develop for you.
If you smoke, it’s a very good idea to quit after a diagnosis of rheumatoid arthritis. This is because:
- rheumatoid arthritis may be worse in smokers than non-smokers
- smoking can weaken how well your medication works.
Physical activity is also important, as it can improve your symptoms and benefit your overall health. The Versus Arthritis website has suitable exercises you can try.
Blood tests and x-rays will help your doctor assess how fast your arthritis is developing and what the outlook for the future may be. This will also help your doctor to decide which treatment
to recommend.
How Frequently patients should come for follow up?
Initially every month and after 3 months once in 3 months as per the guidelines, we follow.
Is there any role of diet?
No food can cause Rheumatoid Arthrities; similarly no strong evidence is ther that any diet can control Rheumatoid Arthrities significantly; however, Omega 3 fatty acid present in fish, has got a mild proactive tole against inflammation, as well as againest Cardiovasular complications. Most spices in indian diet have positive benifit in inflammation. Restrict saturated fat.
Is it hereditary?
It is not fully hereditary, however, there is a likelihood that some of the offsprings of patients with Rheumatoid Arthrities may have some form of autoimmune disease.
Is there any role of alternative system of Medicine?
As far as evidence-based medicine goes, there is no data to support this. In fact, unpredictable harm done by the unknown agents is often that you see Including heavy metal poisoning, crude steroids related toxicity, bone marrow suppression, renal failure, neurotoxicities. These are often noticed in patients taking so-called ‘natural therapy’ and can pose confusion pictures for the treating physician. Don’t be a victim of unscientific traditional medicines.
Do the drugs used in Scientific medicines have the side effects?
Yes , There are no medicines without side effects; but all side effects by the scientific medications in Rheumatoid arthritis are known to us and we can monitor them before any major side effects can happen. Also you should know that all forms of medications including traditional ones have side effects & can be unpredictable in traditional medicines.
What are the other modalities of treatment apart from drug therapy?
Short term benefit with intra articular steroids, short term courses of NSAIDS (Non- Steriodal Anti Inflammatory Drugs) are also needed at times especially during active phase of disease. There is important role of physiotherapy, occupational therapy, Podiatrist and in advanced disease with damage, joint replacement has got very good role to play to improve the quality of life. Joint replacement surgeries are safe & effective.
Living with rheumatoid arthritis
Aids and adaptations
If you have trouble doing everyday tasks, you may find it useful to use certain aids and adaptations.
Aids can help you manage everyday tasks such as bathing,
dressing, and cooking. These can include shoe horns, rails or handles, and shower seats.
Adaptations are bigger items that can help you move around your home. These items include wheelchairs, fixed ramps and baths with built-in handles.
Occupational therapy
Occupational therapists can help you keep doing the activities you need or want to do – at home or at work. They will work with you to find different ways of doing things.
The benefits of seeing an occupational therapist include:
- improved confidence
- being able to do more things, at home or at work
- being able to live independently at home
- allowing you to return to or stay in work.
Managing Symptoms
Flare-ups
When your symptoms get worse, this is known as a flare-up.
These can happen at any time, but can occur after you have been stressed or had an infection.
Over time, you may get better at noticing the early signs of a flare-up.
If you’re having regular flare-ups, you should mention this to your doctor. It may be that you need to review your treatment.
Here are a few things you can do to help yourself during a flare-up:
- Keep taking your medication at the doses you’ve been prescribed.
- Do gentle exercises.
- Put heated items on your joints – these can include a hot water bottle or electric heat pad.
- Put cold items on your joint – these can include a bowl of cold water with ice cubes, a pack of frozen peas wrapped in a towel, or a damp towel that has been kept in the fridge.
Physical activity
Keeping physically active can improve your rheumatoid arthritis symptoms, including pain.
You may find it difficult to be physically active in the first place, especially if you are having a flare-up. However, if you find the right activities, help and support, you can be active in a way that suits you.
Not keeping active can lead to stiff joints and weak muscles. It could also cause you to gain weight.
If you are new to exercise, or haven’t exercised in some time, you may feel a bit sore the first few times you try a new activity. As you
get used to it, this will get better.
Physiotherapy
A physiotherapist can suggest suitable exercises for you and support you in keeping active.
People with rheumatoid arthritis should have access to specialist physiotherapy to help manage their condition and improve their fitness, flexibility and strength. You should also have follow-up reviews.
Hydrotherapy
You may also find that hydrotherapy helps to ease your symptoms. This involves doing special exercises in a warm water pool, under
the supervision of a trained physiotherapist. Hydrotherapy can also be called ‘aquatic therapy’ or ‘aquatic physiotherapy’.


